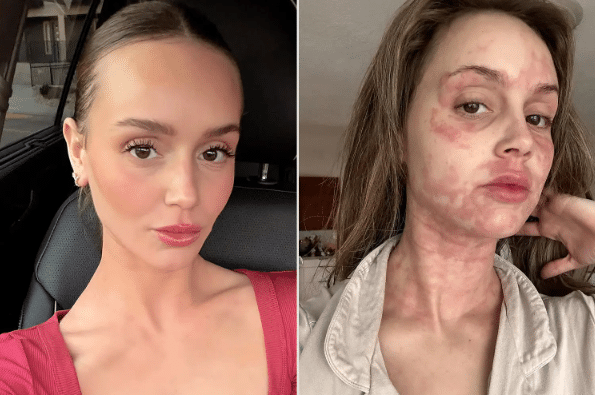
Mast Cell Activation Syndrome (MCAS) can be difficult to recognize because its symptoms often affect multiple parts of the body at the same time. Patients frequently experience a wide variety of reactions that appear unrelated at first glance, leading many people to search for answers for years before mast cell involvement is considered.
This wide range of symptoms occurs because mast cells are present throughout the body. These immune cells play an important role in defending against infections, responding to environmental threats, and regulating inflammation. However, when mast cells become overly reactive, they may release inflammatory chemicals inappropriately or excessively.
These chemicals, often called mast cell mediators, include substances such as histamine, prostaglandins, leukotrienes, and cytokines. When released in large amounts or at inappropriate times, these mediators can trigger symptoms across many organ systems.
Dr. Lawrence Afrin is a board-certified hematologist/oncologist who recently wrote a book, “Never Bet Against Occam: Mast
Cell Activation Disease and the Modern Epidemics of Chronic Illness and Medical Complexity. He explains that ” that MCAS is an epidemic with as many as 14 to 17 percent of the US population having MCAS – one out of every six to seven individuals. It has been said that it may take up to 10 years and numerous doctor visits before someone is adequately diagnosed and treated by a knowledgeable physician—or the patient figures it out for themselves!”
Understanding the common symptom patterns associated with MCAS can help patients and practitioners recognize when mast cell activation may be contributing to chronic illness.
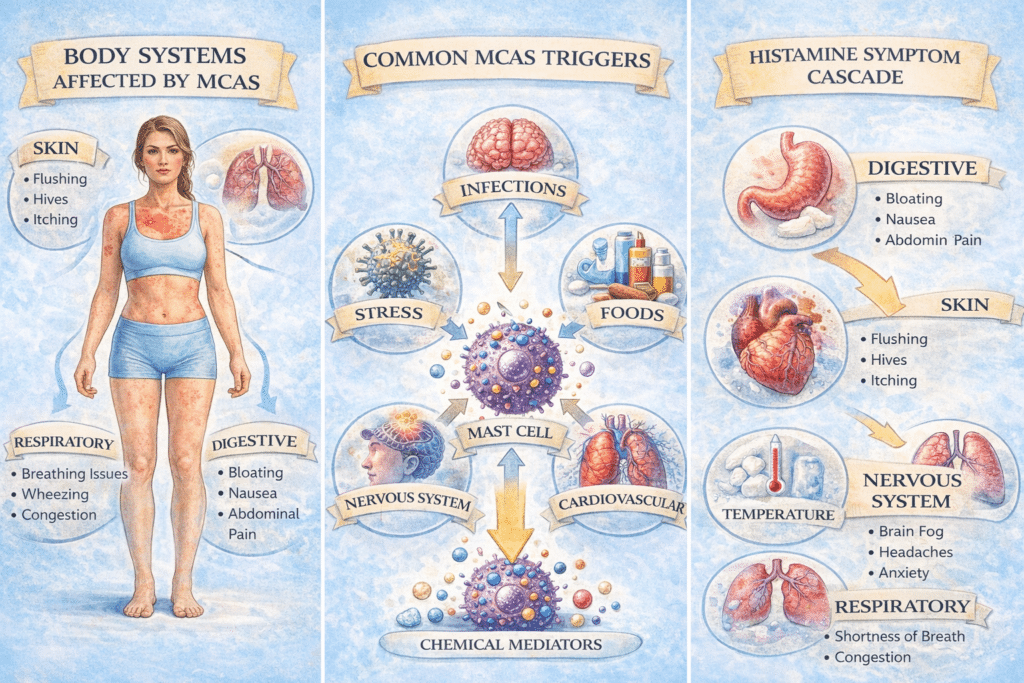
Why Mast Cell Activation Causes So Many Different Symptoms
One of the defining characteristics of mast cell activation syndrome is that symptoms often involve several body systems simultaneously. Unlike conditions that affect only a single organ or tissue, mast cell activation can influence the skin, digestive tract, nervous system, cardiovascular system, and respiratory system.
This occurs because mast cells are widely distributed throughout the body. They are particularly concentrated in areas where the body interacts with the environment, including the skin, lungs, and gastrointestinal tract. Their role is to quickly detect and respond to potential threats.
When mast cells become dysregulated, they may release inflammatory mediators in response to stimuli that would not normally trigger an immune reaction. These responses may be mild or severe and can fluctuate over time.
As a result, individuals with MCAS may notice symptoms that seem unpredictable or triggered by a wide variety of factors. Review the root causes of MCAS.
Many people with these patterns often say, “I’ve felt like this ever since I was a child.” It can show up as being unusually sensitive to things that don’t seem to bother others, like strong reactions to bug bites, medications, or even everyday exposures. Some people notice they have difficulty breathing or feel lightheaded when they stand up. Others recall symptoms starting early in life, like sleep issues, ringing in the ears, frequent infections, or digestive problems as a baby or child.
Over time, this may look like ongoing fatigue, feeling run down, or having symptoms that come and go without a clear pattern. You might notice your body reacts strongly to foods, or smells (especially fragrances), or that you feel inflamed, puffy, or retain fluid at times. Some people experience flushing of the face or chest when stressed, sensitive skin that marks easily, or feel either too cold or intolerant to heat. Healing can feel slower than expected, and there may be a general sense that your body is “overreacting” to the world around you.
Many patients also share a history of frequent illness or infections and may notice swollen lymph nodes at times. Altogether, these symptoms can feel confusing and overwhelming, especially when they’ve been present for so long, but they often point to an underlying pattern that can be understood and supported with the right approach.
Skin Symptoms
Skin reactions are among the most recognizable symptoms of mast cell activation. Because mast cells are abundant in the skin, mediator release can produce noticeable changes in skin appearance and sensation.
Common skin-related symptoms include:
- flushing or sudden redness of the face and neck
- itching or burning sensations
- hives or urticaria
- dermatographia (skin that becomes raised or red when scratched)
- unexplained rashes
- swelling of the lips, eyelids, or face
- cherry angiomata (skin growths)
These symptoms often appear suddenly and may resolve quickly once the inflammatory mediators dissipate. In some individuals, skin reactions may be triggered by heat, stress, foods, medications, or environmental exposures such as mold and VOCs.
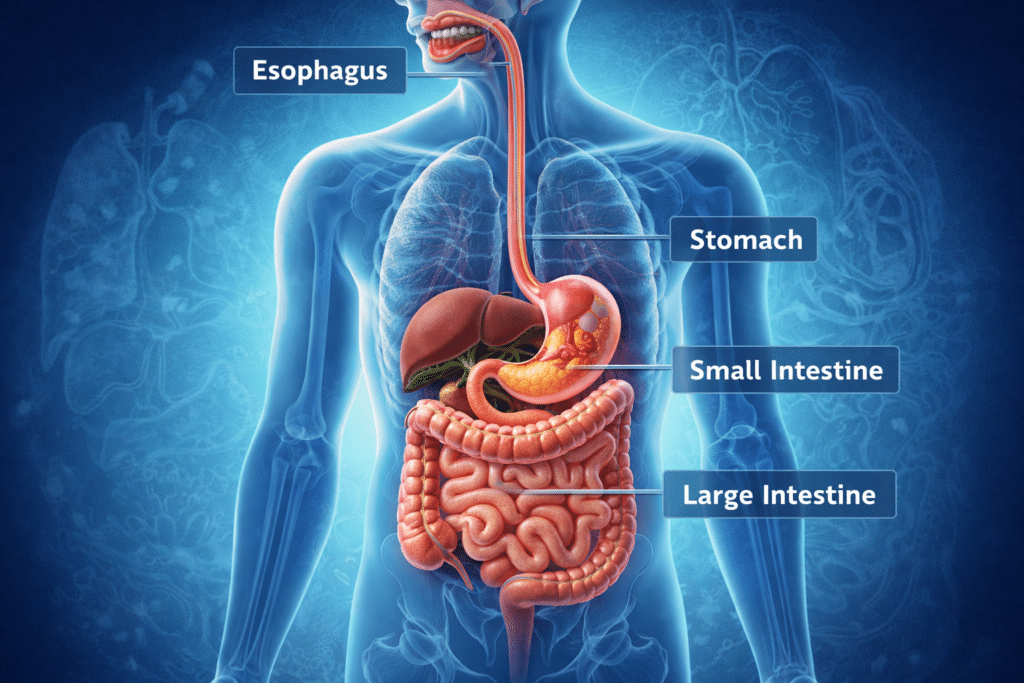
Digestive Symptoms
The gastrointestinal tract contains a large population of immune cells, including mast cells. When mast cells become overactive in the digestive system, a variety of gastrointestinal symptoms can occur.
Common digestive symptoms associated with MCAS include:
- abdominal pain or cramping
- nausea
- diarrhea and/or constipation
- bloating
- acid reflux
- malabsorption
- food sensitivities
Many patients notice that certain foods seem to trigger digestive reactions. These reactions are often related to histamine release or other mast cell mediators affecting the gut.
Digestive symptoms are one reason MCAS is sometimes mistaken for other gastrointestinal conditions before mast cell activation is considered.
Neurological Symptoms
Mast cells also interact closely with the nervous system. The chemicals they release can influence nerve signaling and inflammatory pathways in the brain and peripheral nervous system.
Neurological symptoms may include:
- brain fog or difficulty concentrating
- numbness and tingling
- poor concentration
- headaches or migraines
- dizziness or lightheadedness
- difficulty fining words
- sensitivity to light or sound
- anxiety or sudden mood changes
- attention deficit/hyperactivity disorder (ADHD)
- Insomnia
Because these symptoms overlap with many other conditions, mast cell involvement is often overlooked unless other signs of immune dysregulation are present.
Cardiovascular Symptoms
In some cases, mast cell mediators can affect blood vessels and heart rate regulation. Histamine and other inflammatory chemicals may cause blood vessels to dilate, which can influence circulation and blood pressure.
Cardiovascular symptoms sometimes reported with MCAS include:
- rapid heart rate
- episodes of low and high blood pressure
- palpitations
- dizziness upon standing
- faintness or near fainting
- high triglycerides
- hot flashes
These symptoms sometimes overlap with conditions such as postural orthostatic tachycardia syndrome (POTS), which frequently occurs alongside mast cell activation in individuals with complex chronic illness.
Respiratory Symptoms
Because mast cells are present in the airways, mediator release can also affect breathing and respiratory function.
Respiratory symptoms may include:
- shortness of breath
- throat tightness
- wheezing
- asthma
- air hinger
- nasal congestion
- sinus inflammation
- anaphylaxis
These reactions can sometimes resemble allergic responses, even when traditional allergy testing does not reveal a specific trigger.
Systemic Symptoms
In addition to symptoms affecting specific body systems, mast cell activation can also produce more general systemic symptoms.
These may include:
- chronic fatigue
- temperature sensitivity
- chemical sensitivity
- sleep disturbances
- general feelings of inflammation or malaise
Because mast cell mediators influence many physiological systems, these broader symptoms often accompany the more specific reactions described above.
Additional Common Symptoms
- anemia
- interstitial cystitis
- recurrent or sterile bladder infection
- history of blood clots
- ringing in ears
- popping and fullness in ears
- throat swelling
- difficulty swallowing
Why MCAS Symptoms Often Fluctuate
One of the most confusing aspects of mast cell activation syndrome is the way symptoms can change over time. Patients may experience periods where symptoms are mild or manageable, followed by sudden flares.
This fluctuation occurs because mast cell mediator release is episodic. Certain triggers may increase the likelihood of mast cell activation, while other times the immune system remains relatively stable.
Common triggers may include:
- stress
- infections
- environmental exposures specifically MOLD
- certain foods or medications
- temperature or altitude changes
Identifying patterns and triggers can help patients better understand their symptom cycles.
Why MCAS Symptoms Often Fluctuate Patterns Across Body Systems
When symptoms involve several body systems at once, mast cell activation becomes a possible explanation. While each symptom individually may appear unrelated, the overall pattern can point toward immune dysregulation.
For this reason, clinicians evaluating possible mast cell disorders often look for clusters of symptoms that involve the skin, digestive system, nervous system, and cardiovascular system.
Recognizing these patterns is often the first step in determining whether further evaluation for mast cell activation is appropriate.
When Symptoms Suggest Mast Cell Activation
Because mast cell activation syndrome can mimic many other conditions, diagnosis typically requires careful clinical evaluation along with targeted laboratory testing.
Understanding the range of symptoms associated with mast cell activation can help patients and practitioners consider MCAS as a potential contributor to chronic illness, especially when symptoms affect multiple body systems and fluctuate over time.
Conditions Commonly Associated with MCAS
Mast Cell Activation Syndrome (MCAS) often does not occur in isolation. It is frequently seen alongside other conditions that can both trigger mast cell activation and be worsened by ongoing inflammation.
Some of the most commonly associated conditions include:
- Postural Orthostatic Tachycardia Syndrome (POTS)
- Ehlers-Danlos Syndrome (EDS)
- Chronic Inflammatory Response Syndrome (CIRS), often related to mold exposure
- Small Intestinal Bacterial Overgrowth (SIBO) and gut dysbiosis
- Genetic variations affecting methylation (such as MTHFR), which can impact histamine breakdown
At the core of MCAS is the release of inflammatory mediators, one of the most well-known being histamine. Under normal circumstances, the body has built-in systems to break histamine down and keep it balanced.
These include:
- DAO (diamine oxidase) – helps break down histamine from foods in the gut
- HNMT (histamine-N-methyltransferase) – helps clear histamine within cells, particularly in the liver
- Methylation pathways – support overall histamine metabolism and detoxification
When these systems are not functioning optimally—whether due to genetics, inflammation, or gut dysfunction—histamine can begin to accumulate in the body.
This is especially important in the gut. If there is SIBO or dysbiosis, the intestinal lining can become irritated and compromised. This can lead to:
- Reduced DAO enzyme production
- Increased intestinal permeability (“leaky gut”)
- Greater absorption of histamine and other inflammatory compounds
As a result, a cycle can develop where histamine drives inflammation, and inflammation further impairs the body’s ability to break histamine down.
In conditions like POTS and Ehlers-Danlos Syndrome, this becomes even more relevant. Many patients with these conditions have underlying connective tissue and nervous system sensitivities that can make them more prone to mast cell activation, histamine intolerance, and systemic inflammation.
Understanding these interconnected patterns is key, as addressing MCAS often requires a whole-body approach. Supporting the gut, improving detoxification pathways, and calming the immune system to help restore balance is key in the recovery process.