Understanding MCAS Treatment
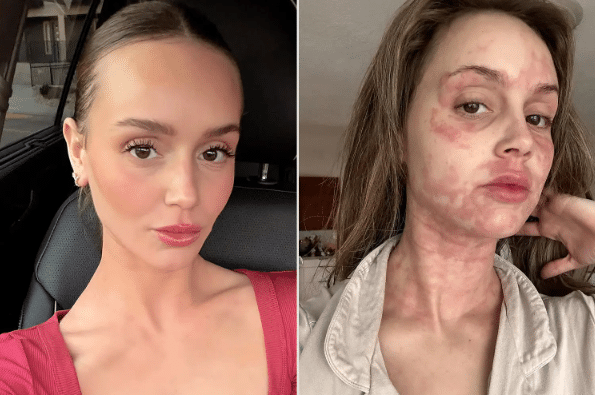
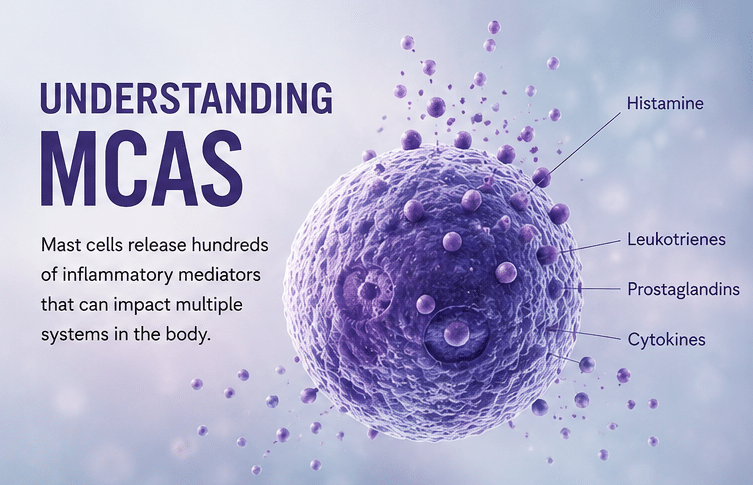
Mast Cell Activation Syndrome (MCAS) is a complex, multisystem condition that often requires a highly individualized treatment approach. Mast cells release hundreds of inflammatory mediators, including histamine, leukotrienes, prostaglandins, cytokines, and chemokines. Due to these inflammatory mediators, treatment often involves addressing multiple pathways simultaneously while also identifying the root causes driving immune dysregulation.
One of the most important things to understand is that antihistamines do not actually stop mast cells from releasing histamine. Instead, they block histamine receptors and help reduce the symptoms caused by histamine release.
For many individuals with MCAS, symptom management requires around-the-clock blockade of both histamine H1 and H2 receptors, often every 12 hours, in combination with mast cell stabilization, nervous system regulation, gut healing, mitochondria support, and reduction of inflammatory triggers.
Recovery from MCAS is rarely linear. What works well for one person may significantly flare another. In my experience both personally and professionally, one of the biggest keys to success is going low and slow. Introducing therapies gradually, one at a time, allows the body to adapt before layering additional interventions.
At The Lyme Specialist, we help guide individuals through this highly individualized recovery process. MCAS is something I have personally experienced myself, and I understand how overwhelming it can feel trying to determine which therapies help, which worsen symptoms, and how to find the right balance to move healing forward safely.
Our goal is to help patients build a foundation that allows the immune system to become more stable and resilient over time.
Conventional Medications Commonly Used in MCAS Treatments
Treatment plans may include a combination of:
H1 Antihistamines
These block histamine at the H1 receptor and may help symptoms such as itching, flushing, hives, anxiety, insomnia, headaches, and reactivity.
Examples include:
- Hydroxyzine
- Cetirizine (Zyrtec)
- Levocetirizine (Xyzal)
- Loratadine (Claritin)
- Fexofenadine (Allegra)
- Diphenhydramine (Benadryl)
- Ketotifen
- Doxepin
H2 Antihistamines
These help block histamine activity within the gastrointestinal tract and may reduce reflux, nausea, abdominal pain, diarrhea, and systemic histamine burden.
Examples include:
- Famotidine (Pepcid)
- Cimetidine (Tagamet)
Famotidine is often preferred due to fewer drug interactions.
Mast Cell Stabilizers
These therapies aim to reduce mast cell degranulation and inflammatory mediator release.
Examples include:
- Cromolyn sodium
- Ketotifen
- Quercetin
- Hydroxyurea (in select cases)
Leukotriene Inhibitors
These target inflammatory leukotriene pathways involved in respiratory symptoms, inflammation, and mast cell activation.
Examples include:
- Montelukast (Singulair)
- Zafirlukast (Accolate)
Additional Therapies Sometimes Considered
Depending on the individual case, additional therapies may include:
- Low-dose naltrexone (LDN)
- Omalizumab (Xolair)
- IVIG
- Cannabinoids (particularly CBD)
- Benzodiazepines in carefully selected cases
- Tyrosine kinase inhibitors such as Imatinib
Medication dosing and timing vary greatly from person to person, and many patients require extremely gradual titration to avoid flares.

Foundational Integrative Approaches to MCAS Treatment
1. Reducing Histamine Burden Through Diet
A low-histamine diet can help reduce incoming histamine exposure, though it does not directly stop mast cell overactivity.
Common high-histamine foods include:
- Alcohol
- Fermented foods, especially kefir, sauerkraut, and kombucha
- Smoked and cured meats
- Leftovers
- Vinegar
- Aged cheeses
- Tomatoes
- Citrus
- Shellfish
- Strawberries
- Spinach
- Processed foods and preservatives
Many patients notice significant symptom improvement when focusing on fresh, minimally processed foods and avoiding leftovers.
2. Supporting Histamine Breakdown (DAO)
Diamine oxidase (DAO) is one of the primary enzymes responsible for breaking down histamine.
DAO support may include:
- DAO enzyme supplementation before meals
- Vitamin C
- Gut healing support
- Reducing alcohol intake, as alcohol inhibits DAO activity
Alcohol can be particularly problematic in MCAS because it both triggers histamine release and impairs histamine breakdown simultaneously.
3. Natural Mast Cell Stabilizers
Several nutrients and botanical compounds have demonstrated mast cell stabilizing and anti-inflammatory properties.
Commonly used supplements include:
- Quercetin
- Vitamin C
- Curcumin
- EGCG (green tea extract)
- Luteolin
- Resveratrol
- Omega-3 fatty acids
- Magnesium
- NAC
- Alpha lipoic acid
- Selenium
- Nigella sativa
- Ginger
- Turmeric
- Lemon balm
- Stinging nettle
Quercetin is one of the most widely used natural mast cell stabilizers and may help inhibit the release of histamine, prostaglandins, and leukotrienes.
However, it is important to recognize that not every “mast cell stabilizer” works well for every individual. Genetics, detoxification capacity, nervous system regulation, and overall biochemical individuality can significantly impact tolerance.
For example, some individuals with variations in the COMT gene may be more sensitive to compounds such as Quercetin and EGCG. The COMT enzyme plays an important role in breaking down catecholamines such as dopamine, norepinephrine, and epinephrine, along with certain polyphenols. In some individuals, these compounds may slow COMT activity further, potentially contributing to symptoms like feeling overstimulated, anxious, “wired,” or having difficulty sleeping.
Personally, I have experienced this reaction with quercetin due to SNPs affecting my COMT pathway, which is a reminder that even natural supplements can have very individualized effects depending on a person’s genetics and biochemistry.

4. Nervous System Regulation and Limbic System Retraining
The nervous system plays a major role in mast cell activation and immune regulation. Many individuals with MCAS have been living in a prolonged state of sympathetic nervous system activation, commonly referred to as “fight-or-flight.”
When the nervous system perceives danger continuously — whether from chronic illness, infections, mold exposure, trauma, environmental triggers, or ongoing physiological stress — the body may remain stuck in a heightened inflammatory state. Over time, this can contribute to:
- Increased mast cell activation
- Heightened histamine responses
- Chemical and food sensitivities
- Hypervigilance
- Adrenal dysfunction
- Sleep disturbances
- Digestive dysfunction
- Increased reactivity to supplements, medications, and environmental exposures
Mast cells and the nervous system communicate closely with one another. Stress hormones and nervous system signaling can directly influence mast cell degranulation, while inflammatory mediators released by mast cells can further stimulate the nervous system, creating a self-perpetuating cycle.
For many individuals, nervous system regulation becomes a critical component of reducing overall reactivity and improving treatment tolerance.
Therapies that may help support nervous system regulation include:
- Limbic system retraining programs
- Breathwork
- Somatic therapy
- Vagus nerve support
- Meditation and mindfulness practices
- Trauma-informed therapy
- Gentle movement
- Nature exposure
- Brain retraining techniques
- Sleep optimization
- Reducing overstimulation and stress load
At The Lyme Specialist, we often emphasize that healing is not simply about killing pathogens or suppressing symptoms. It is also about helping the body feel safe enough to shift out of survival mode and back into a state that supports regulation, repair, and resilience.
In my experience, some of the most sensitive patients are not only dealing with biochemical and inflammatory imbalances, but also deeply dysregulated nervous systems that have been under chronic stress for years. Supporting the nervous system alongside the immune system can often be one of the missing links in helping patients tolerate treatment and move healing forward more sustainably.
Addressing Root Causes of Mast Cell Activation
In many cases, MCAS is not occurring in isolation.
Potential underlying triggers may include:
- Chronic infections
- Lyme disease and co-infections
- Mold exposure and biotoxins
- Chemical exposures
- Gut dysbiosis
- Environmental toxins
- Heavy metals
- Nervous system dysregulation
- Chronic stress
- Autoimmune activation
At The Lyme Specialist, we focus heavily on identifying and addressing these upstream contributors while simultaneously stabilizing the body enough to tolerate deeper healing work.
This often includes:
- Supporting drainage and detoxification pathways
- Nervous system regulation
- Gut restoration
- Mitochondrial support
- Environmental assessments
- Reducing inflammatory burden
- Building resilience before aggressive therapies are introduced
T-Regulatory Cell (Treg) Therapy and Immune Regulation
Emerging therapies aimed at restoring immune regulation are creating new possibilities for individuals with severe immune dysregulation, chronic inflammation, and treatment-resistant chronic illness.
One area of growing interest involves T-regulatory cell (Treg) therapies centered around FOXP3, the master regulatory protein that governs Treg cell function.
In chronic conditions, FOXP3 signaling may become unstable or impaired. When this occurs, the immune system can become overactive, misdirected, and unable to properly regulate inflammatory responses. This loss of immune balance may contribute to persistent inflammation, hypersensitivity reactions, mast cell activation, autoimmune tendencies, and difficulty tolerating treatment.
We partner with a hospital that offers advanced Treg therapy designed specifically for patients with chronic immune dysregulation.
This therapy involves:
- Collecting the patient’s own T cells
- Engineering them with stabilized FOXP3 expression
- Stress-testing the cells in laboratory conditions designed to replicate chronic inflammatory environments
- Selecting the most resilient regulatory cells
- Expanding and reinfusing them back into the patient
The goal is to help restore immune regulation at a foundational level and improve the body’s ability to calm chronic inflammatory signaling. Treg therapy represents an exciting frontier in immune modulation and precision medicine.
The Importance of Individualized Care
MCAS treatment is rarely about finding a single “magic bullet.” Diagnosis is one thing but treatment and further than that, healing, is another.
Healing often requires:
- careful pacing
- strategic layering of therapies
- nervous system support
- identifying triggers
- stabilizing inflammation
- and building tolerance gradually over time
For many individuals, the biggest breakthroughs in MCAS treatment happen not from doing more, but from learning how to support the body in a way that feels safe, sustainable, and personalized.
This condition can be incredibly isolating and discouraging, especially for those who have spent years searching for answers. But with the right support, individualized care, and a thoughtful approach, improvement is possible.